Opening hours
| Monday-Thursday | 08:00 - 18:00 |
| Friday | 08:00 - 17:00 |
| Saturday | Closed |
| Sunday | Closed |
Contact
Hypertension
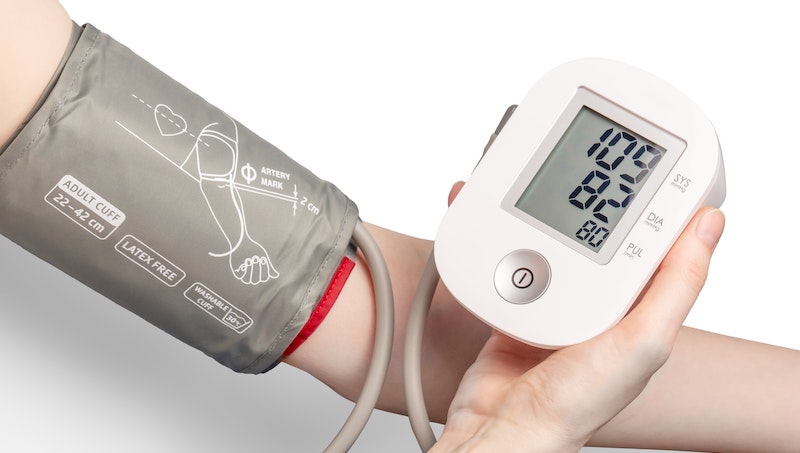
Hypertension, also referred to as high blood pressure, HTN or HPN, is a medical condition in which the blood pressure is chronically elevated. In current usage, the word "hypertension"without a qualifier normally refers to systemic, arterial hypertension.
Hypertension can be classified either essential (primary) or secondary. Essential hypertension indicates that no specific medical cause can be found to explain a patient's condition. Secondary hypertension indicates that the high blood pressure is a result of (i.e., secondary to) another condition, such as kidney disease or tumours (pheochromocytoma and paraganglioma).
Persistent hypertension is one of the risk factors for strokes, heart attacks, heart failure and arterial aneurysm, and is a leading cause of chronic renal failure. Even moderate elevation of arterial blood pressure leads to shortened life expectancy. At severely high pressures, defined as mean arterial pressures 50% or more above average, a person can expect to live no more than a few years unless appropriately treated. Beginning at a systolic pressure of 115 mm Hg and diastolic pressure of 75 mm Hg (commonly written as 115/75 mm Hg), cardiovascular disease (CVD) risk doubles for each increment of 20/10 mm Hg. In the United States, prehypertension is defined as blood pressure from 121/81 mm Hg to 139/89 mm Hg and although not a disease category, it is a designation chosen to identify individuals at high risk of developing hypertension.The Mayo Clinic specifies that blood pressure is normal if it is 120/80 mm Hg or below.
In individuals older than 50 years, hypertension is considered to be present when a person's blood pressure is consistantly at least 140 mm Hg systolic or 90 mm Hg diastolic. Patients with blood pressures over 130/80 mm Hg along with Type 1 or Type 2 diabetes, or kidney disease require further treatment.
Resistant hypertension is defined as the failure to reduce BP to the appropriate level after taking a three-drug regimen. Guidelines for treating
CAUSES
Essential (primary) hypertension
By definition, essential hypertension has no identifiable cause. However, several risk factors have been identified, including obesity, salt sensitivity, renin homeostasis, insulin resistance, genetics, and age.
Obesity
The risk of hypertension is 5 times higher in the obese as compared to those of normal weight and up to two-thirds of cases can be attributed to excess weight. More than 85% of cases occur in those with a Body mass index greater than 25.[8]A definitive link between obesity and hypertension has been found using animal and clinical studies, from these it has been realised that many mechanisms are potential causes of obesity induced hypertension.These mechanisms include the activation of the sympathetic nervous system as well as the activation of the renin-angiotensin-aldosterone system.[9]
Sodium sensitivity
Sodium is an environmental factor that has received the greatest attention. Approximately one third of the essential hypertensive population is responsive to sodium intake.[10] This is because increasing the amount of salt in a person's bloodstream causes cells to release water (due to osmotic pressure) to equilibrate the concentration gradient between the cells and the bloodstream, thereby increasing the pressure within the blood vessel walls[citation needed]. The increased Na+ stimulates ADH and thirst mechanisms, leading to a concentrated urine and the kidneys holding onto water along with the person increasing the intake of water. Also, the water movement between cells and the interstitium plays a minor role compared to this.
Role of renin
Renin is an enzyme secreted by the juxtaglomerular apparatus of the kidney and linked with aldosterone in a negative feedback loop. The range of renin activity observed in hypertensive subjects tends to be broader than in normotensive individuals. In consequence, some hypertensive patients have been defined as having low-renin and others as having essential hypertension. Low-renin hypertension is more common in African Americans than white Americans, and may explain why African Americans tend to respond better to diuretic therapy than drugs that interfere with the Renin / angiotension system.
How high renin levels predispose to hypertension: Increased renin ? Increased angiotensin II ? Increased vasoconstriction, thirst/ADH and aldosterone ? Increased sodium resorption in the kidneys (DCT and CD) ? Increased blood pressure.
Some authorities claim that potassium might both prevent and treat hypertension.
Insulin resistance
Insulin is a polypeptide hormone secreted by cells in the islets of Langerhans, which are contained throughout the pancreas. Its main purpose is to regulate the levels of glucose in the body antagonistically with glucagon through negative feedback loops. Insulin also exhibits vasodilatory properties. In normotensive individuals, insulin may stimulate sympathetic activity without elevating mean arterial pressure. However, in more extreme conditions such as that of the metabolic syndrome, the increased sympathetic neural activity may over-ride the vasodilatory effects of insulin. Insulin resistance and/or hyperinsulinemia have been suggested as being responsible for the increased arterial pressure in some patients with hypertension. This feature is now widely recognized as part of syndrome X, or the metabolic syndrome.
Genetics
Hypertension is one of the most common complex disorders.The etiology of hypertension differs widely amongst individuals within a large population.
Hypertension may be secondary to other diseases but over 90% of patients have essential hypertension which is of unknown origin. It is observed though that:
- Having a personal family history of hypertension increases the likelihood that an invividual develops HPT.
- Essential hypertension is four times more common in black than caucasian peoples, accelerates more rapidly and is often more severe with higher mortality in black patient.
More than 50 genes have been examined in association studies with hypertension, and the number is constantly growing.One of these gene is angiotensinogen (AGT) gene, studied extensively by Kim et al. They showed that increasing the number of AGT increases the blood pressure and hence this may cause hypertension.Twins have been included in studies measuring ambulatory blood pressure, from these studies it has been suggested that essential hypertension contains a large genetic influence.Supporting data has emerged from animal studies as well as clinical studies in human populations.The majority of these studies support the concept that the inheritance is probably multifactorial or that a number of different genetic defects each have an elevated blood pressure as one of their phenotypic expressions.However, the genetic influence upon hypertension is not fully understood at the moment. It is believed that linking hypertension-related phenotypes with specific variations of the genome may yield definitive evidence of heritability.
Another view is that hypertension can be caused by mutations in single genes, inherited on a mendelian basis.
Age
Hypertension can also be age related, if this is the case it is likely to be multifactorial. One possible mechanism involves a reduction in vascular compliance due to the stiffening of the arteries. This can build up due to isolated systolic hypertension with a widened pulse pressure. A decrease in glomerular filtration rate is related to aging and this results in decreasing efficiency of sodium excretion. The developing of certain diseases such as renal microvascular disease and capillary rarefaction may relate to this decrease in efficiency of sodium excretion. There is experimental evidence that suggests that renal microvascular disease is an important mechanism for inducing salt-sensitive hypertension.
PREVENTION
The degree to which hypertension can be prevented depends on a number of features including: current blood pressure level, changes in end/target organs (retina, kidney, heart - among others), risk factors for cardiovascular diseases and the age at presentation. Unless the presenting patient has very severe hypertension, there should be a relatively prolonged assessment period within which should be repeated measurements of blood pressure. Following this, lifestyle advice and non-pharmacological options should be offered to the patient, before any initiation of drug therapy.
The process of managing hypertension according the the guidelines of the British Hypertension Society suggest that non-pharmacological options should be explored in all patients who are hypertensive or pre-hypertensive. These measures include;
Weight reduction and regular aerobic exercise (e.g., walking) are recommended as the first steps in treating mild to moderate hypertension. Regular exercise improves blood flow and helps to reduce resting heart rate and blood pressure. Several studies indicate that low intensity exercise may be more effective in lowering blood pressure than higher intensity exercise. These steps are highly effective in reducing blood pressure, although drug therapy is still necessary for many patients with moderate or severe hypertension to bring their blood pressure down to a safe level.
Reducing dietary sugar intake
Reducing sodium (salt) in the diet may be effective: It decreases blood pressure in about 33% of people (see above). Many people use a salt substitute to reduce their salt intake.
Additional dietary changes beneficial to reducing blood pressure includes the DASH diet (dietary approaches to stop hypertension), which is rich in fruits and vegetables and low-fat or fat-free dairy foods. This diet has been shown to be effective based on research sponsored by the National Heart, Lung, and Blood Institute. In addition, an increase in daily calcium intake has the benefit of increasing dietary potassium, which theoretically can offset the effect of sodium and act on the kidney to decrease blood pressure. This has also been shown to be highly effective in reducing blood pressure.
Discontinuing tobacco use and alcohol consumption has been shown to lower blood pressure. The exact mechanisms are not fully understood, but blood pressure (especially systolic) always transiently increases following alcohol or nicotine consumption. Besides, abstention from cigarette smoking is important for people with hypertension because it reduces the risk of many dangerous outcomes of hypertension, such as stroke and heart attack. Note that coffee drinking (caffeine ingestion) also increases blood pressure transiently but does not produce chronic hypertension.
Reducing stress, for example with relaxation therapy, such as meditation and other mindbody relaxation techniques, by reducing environmental stress such as high sound levels and over-illumination can be an additional method of ameliorating hypertension. Jacobson's Progressive Muscle Relaxation and biofeedback are also used, particularly, device-guided paced breathing, although meta-analysis suggests it is not effective unless combined with other relaxation techniques.
